Anesthesia For Cats
Anesthesia for cats is a wonderful thing! Just imagine how many medical and surgical procedures we couldn’t do without it! Contemplating general anesthesia for your cat can also feel a bit scary. There are so many questions: what does general anesthesia mean? Is all general anesthesia the same? How do I assess any particular risks my cat might have? How do I avoid or minimize those risks? What kinds of problems might happen? How common are these problems? Why are anesthesia costs what they are? Will my cat be the same after a full general anesthetic event?
If you are asking any of these questions, you’re not alone. In this article, we will take a look at anesthesia for cats in general, and we’ll answer a bunch of these questions.
General anesthesia for cats can be thought of as one end of the “spectrum of sedation”
Why Does My Cat Need General Anesthesia?
General anesthesia for cats is indispensable for many kinds of procedures for multiple reasons. For any procedure or test where pain or discomfort is induced, unconsciousness is clearly desirable. Immobilization of the patient is necessary for most surgical procedures, and for some diagnostic tests, such as any radiographs for which the level of detail needed means that no motion artifact can be tolerated. Many procedures, such as dental cleaning, cannot be performed effectively in cats without general anesthesia.
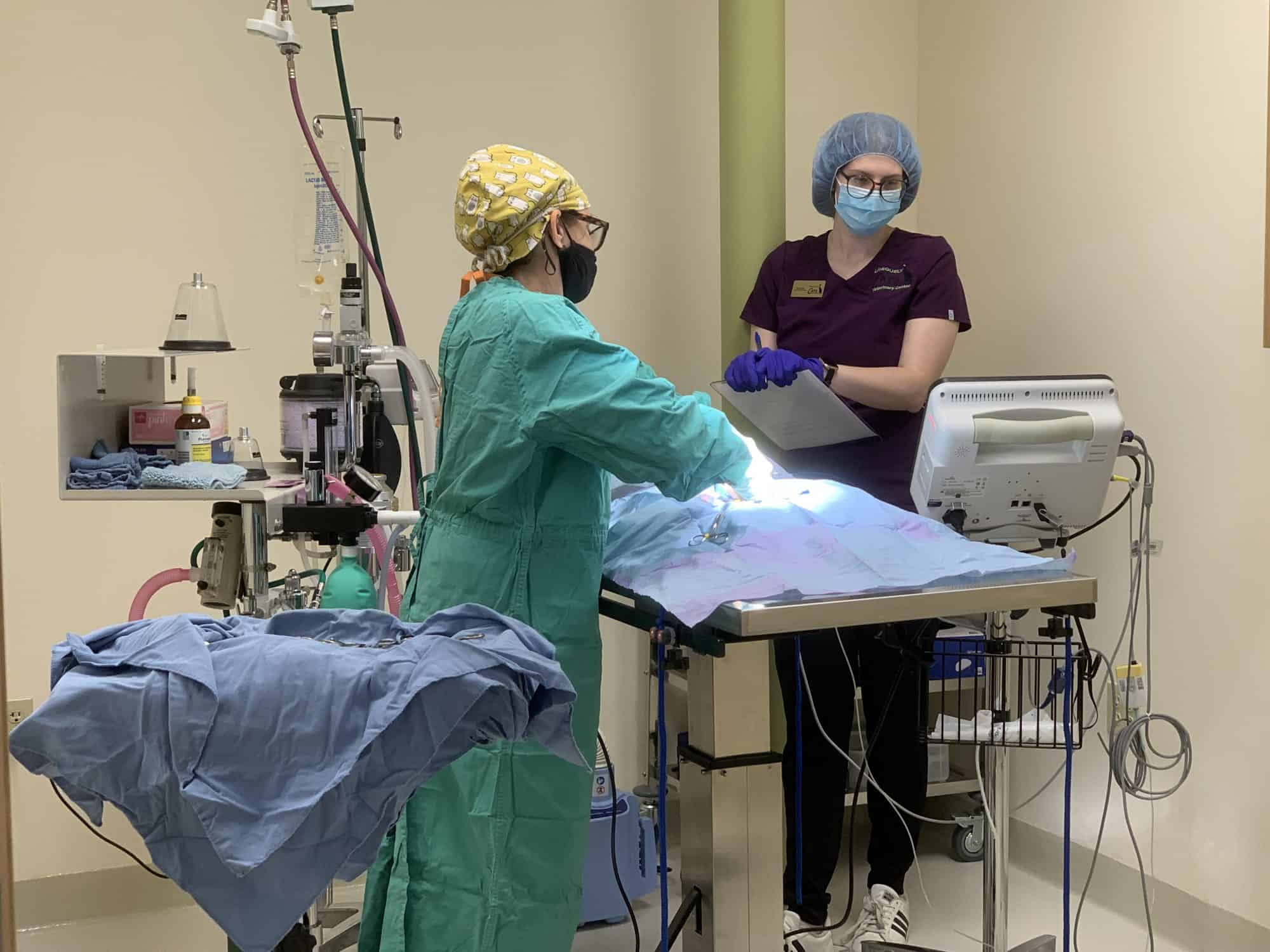
What Does Feline General Anesthesia Mean?
Feline general anesthesia is defined as a state of unconsciousness induced by drugs, affecting the whole body. Under general anesthesia, a cat is not arousable even by a painful stimulus such as surgery. An endotracheal tube is usually placed to deliver oxygen and anesthetic gases. IV fluids are usually given, to maintain good circulation and to provide a route of administration for any drugs your cat may need. Good management of feline general anesthesia requires a dedicated team member to monitor and record vital signs every few minutes and to monitor and manage the depth of anesthesia.
The “Spectrum Of Sedation”
General anesthesia for cats can be thought of as one end of the “spectrum of sedation,” which ranges from a small dose of an anxiety-relief medication (which leaves the patient fully awake), through several intermediate stages, all the way to full general anesthesia. The degree of sedation/anesthesia needed depends on the procedure in question, and may depend as well on the individual cat. There are many procedures that always require full general anesthesia; for cats, any general surgery or dental work requires general anesthesia.
All General Anesthesia For Cats Is Not The Same
There are many ways to perform general anesthesia for a cat. Often, combinations of drugs are used to induce and/or maintain anesthesia; this “multimodal” approach is valuable because it minimizes the risks of side effects of any one drug, and because these drugs may work synergistically. Once general anesthesia has been “induced” (started) in a cat, it may be maintained with the administration of an anesthetic gas, or by a constant rate of IV drug infusion or both.
Not all procedures require all elements of general anesthesia. Very short procedures, such as a punch skin biopsy or a minor wound debridement, may sometimes be performed well and safely with neither an IV catheter nor an endotracheal tube, although anesthetic monitoring requirements remain the same. Higher-risk patients may still require both for optimal safety.
Before General Anesthesia For Your Cat
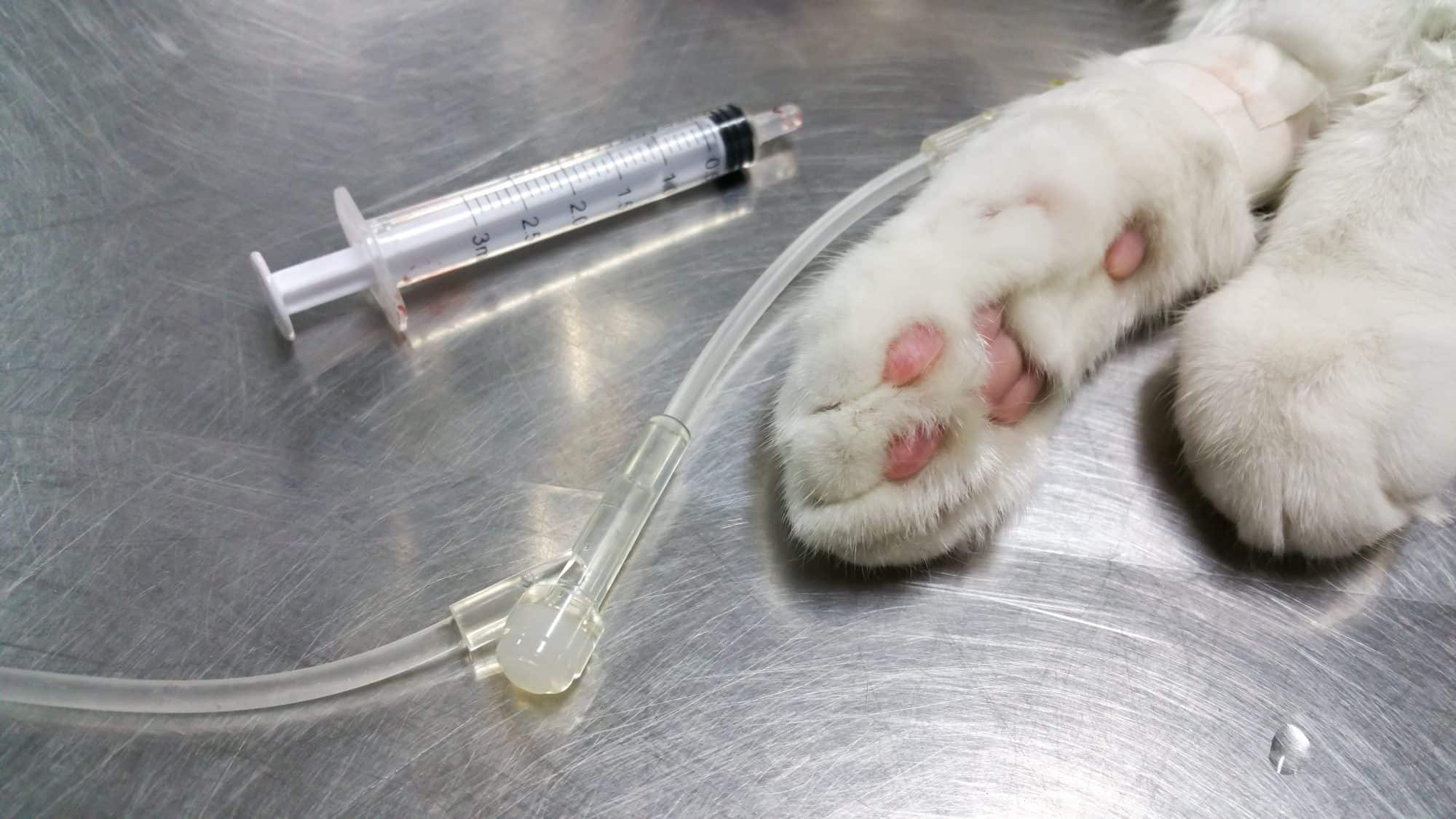
Ask About Your Hospital’s Routines
Anesthetic Drug Protocols: Each veterinary hospital may perform anesthesia for cats differently. Some may use only one drug rather than a combination. Some may not routinely place an IV catheter or an endotracheal tube (these are very important in the event of a problem during anesthesia). Some may choose drugs that can be reversed quickly in order to be able to do more procedures, rather than recovering a patient slowly and without a shock to the system. A hospital may or may not incorporate analgesics (pain relief) and anti-inflammatory drugs into the anesthetic premedication, and may or may not use local or regional anesthesia (that Novocaine shot at the dentist is a great example of a regional anesthetic) in addition to general anesthesia. These choices are all important to minimize anesthetic risk and post-operative discomfort. As a devoted cat parent, you need to know what your hospital’s feline general anesthesia practices are.
Analgesics: Most anesthetic drugs do not provide analgesia (there are some exceptions). Without analgesia, an anesthetized patient still experiences and responds to pain, even though they are not consciously aware of it. When pain is present, more anesthesia is needed to keep the patient unconscious, which increases anesthetic risk. Ideally, an analgesic is incorporated in the anesthetic pre-medication, to stop pain before it can start. Analgesics may be given throughout a procedure when indicated and can be dispensed for home treatment after the procedure. Local and regional anesthetic blocks can be very helpful too, reducing the needed doses of both anesthetics and analgesics, and thereby reducing overall risk.
Anti-inflammatory Treatment: It has recently become understood that inflammation is an inextricable part of the phenomenon of pain. Inflammation is an unavoidable part of any surgical procedure, but can be minimized in several ways. One important method is to incorporate an anti-inflammatory medication into the anesthetic premedication protocol. Gentle surgical techniques and well-maintained instruments can minimize inflammation. Postoperative treatment with cold laser therapy, PEMF (Pulsed Electromagnetic Field) therapy, and even old-fashioned things like warm and cold packs can help significantly to reduce and minimize inflammation, and therefore pain as well.
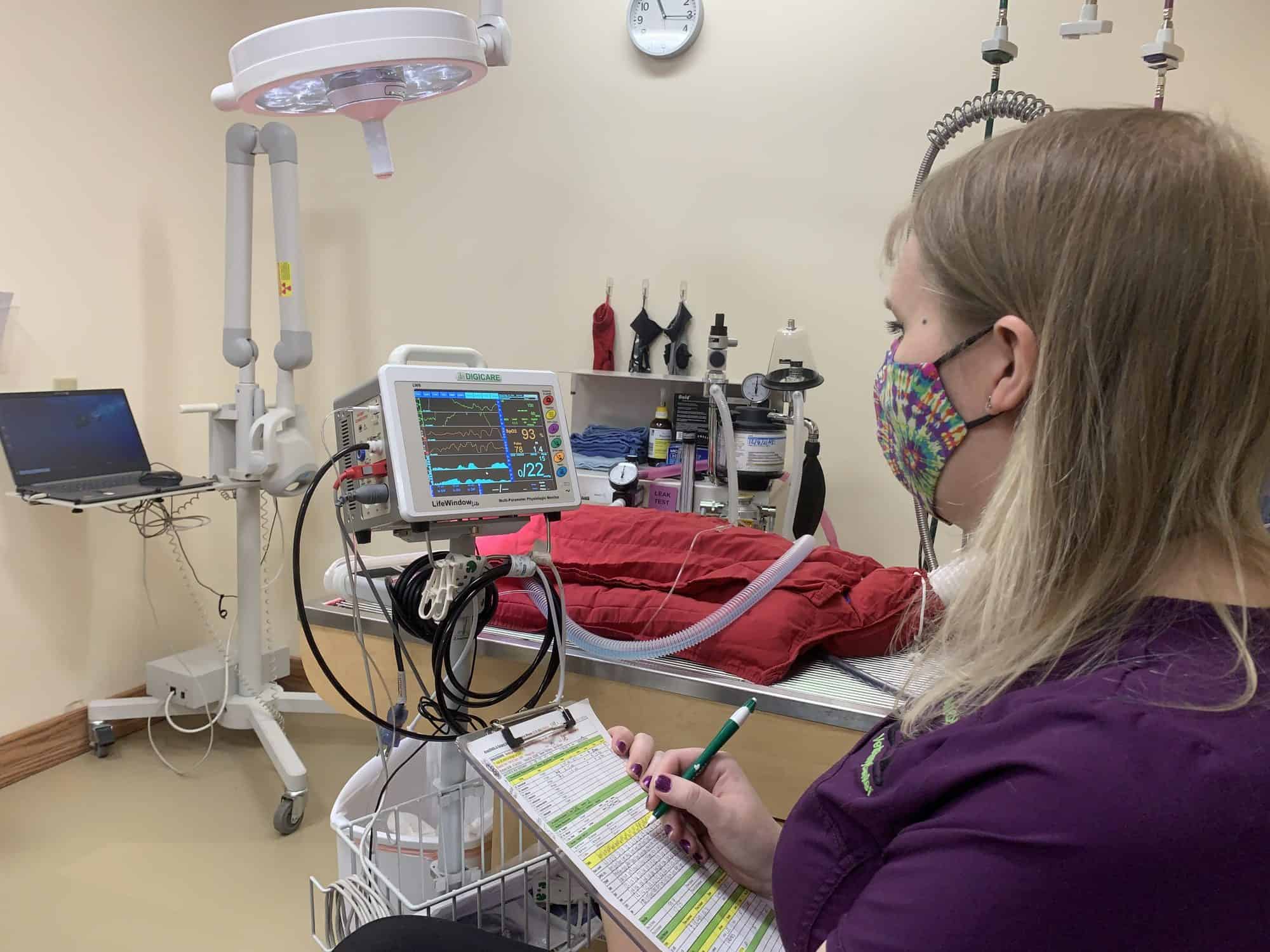
Ancillary Support: Anesthesia for cats is not just about the drugs that are used. Ancillary support is crucial, so you will want to understand your hospital’s ancillary support practices as well. Many cats will lose body heat quickly under anesthesia, which is undesirable; anesthetic outcomes are strongly influenced by the maintenance of normal body temperature. At Uniquely Cats Veterinary Center, heat support is provided, and body temperature is monitored throughout any anesthetic procedure. Some hospitals may not have a technician monitoring vital signs. At UCVC, all vital signs are monitored, including blood pressure, blood oxygen saturation, heart rate and rhythm, respiratory rate, and more by a technician focused solely on the cat. Our anesthetic protocols are designed to avoid problems in these areas, but we are always prepared to address any unexpected problems that may arise.
Feline Anesthesia Recovery: The anesthetic recovery period should be closely monitored; anesthetic complications can occur even while the patient is waking up. At UCVC, once your kitty’s surgical procedure is completed, he or she is placed in fleece recovery bags and cradled in the arms of a technician throughout recovery. This helps keep the patient warm and ensures close monitoring during the recovery period.
Assessing Your Cat For Anesthetic Competency
Ideally, any patient for whom feline general anesthesia is contemplated should be assessed for anesthetic risks. A good anesthetic assessment will be tailored to your cat’s medical history, age, current known problems, current physical state, and so on.
Tailoring An Anesthetic Assessment to Your Cat
For a young, apparently healthy cat with no known disorders, a comprehensive anesthetic risk assessment may consist of an examination, history review, and a basic general laboratory profile (CBC, biochem profile, and urinalysis, as an example). For Senior cats, who are at higher risk of having unidentified disorders, more extensive laboratory screening, including thyroid function testing, is likely to be indicated.
For cats with specific health concerns, specific diagnostic tests may be indicated to assess those concerns. For instance, if your kitty has a heart murmur or arrhythmia, an echocardiogram may be indicated to assess heart function before anesthesia. For some patients, pre-anesthetic screening may include radiographs of the chest and/or abdomen. Your cat vet may recommend additional diagnostic testing based on your cat’s age, health status, history, or examination results.
Understanding your cat’s physical strengths and weaknesses before anesthesia can help your cat veterinarian design the safest possible anesthetic plan for your cat.
How Does An Anesthetic Assessment Help My Cat?
Risk Assessment and Mitigation: Just as in humans, general anesthesia for cats always carries risks, up to and including death. These risks can be mitigated when a patient is assessed thoroughly beforehand. Understanding your cat’s physical strengths and weaknesses before anesthesia can help your cat veterinarian design the safest possible anesthetic plan for your cat. When anesthesia for cats is planned and performed well, risks can be minimized and anesthesia can be quite safe, although individual outcomes can never be guaranteed.
All anesthetic drugs “put some pressure” on various organs. Anesthetic drug protocols can be designed to accommodate or circumvent any particular weakness your cat may have. The following examples briefly describe two common challenges and some ways to mitigate associated risks:
Example 1 — Renal Insufficiency: For instance, if your cat has some loss of renal function, anesthetic drugs to be considered may include medications that are metabolized and excreted by the liver rather than the kidneys; and because the kidneys are exquisitely sensitive to blood oxygen levels, special additional medications may be used to maintain blood pressure above a certain point to keep that oxygen delivery level high.
Example 2 — Heart Disease: If your cat has a mild heart disorder, drug choices may include anesthetics known to cause only minimal cardiovascular suppression (all anesthetic drugs have some cardiovascular suppressive effect); and IV fluid rates may be kept low in order to avoid overloading the heart’s pumping ability.
Except in rare cases, the question isn’t “can my cat have anesthesia,” but rather “what is the safest way to perform anesthesia for my cat?” Answering this question is the aim of a good anesthetic assessment.
Feline General Anesthetic Costs versus Risks
As you can see, it is possible to induce anesthesia with a single drug and no support or monitoring, which can be inexpensive. However, the tradeoff for the low price is an increased risk of complications, pain, and even death. Full feline general anesthesia performed after a full individual patient assessment, with well-tailored protocols, full ancillary support, close monitoring, and good recovery practices, requires a great deal of costly equipment, well-trained personnel, many supplies and medications, and a good deal of doctor time. Providing this level of care carries a higher cost than lesser levels of care have, but higher levels of care come with less risk and better likely outcomes. The equation is essentially a cost/risk/benefit assessment, and only you can decide how much risk you feel comfortable with for your fur baby.
In summary, general anesthesia for cats is never entirely risk-free, but your hospital’s practices can make a huge difference in the level of risk for your cat; and when done well, anesthesia can be very safe. But caveat emptor! Different anesthetic protocols are not all equally good or equally safe. Be sure you understand your hospital’s practices before you decide what is right for your cat.


